New funding to help crack Australia’s high blood pressure problem
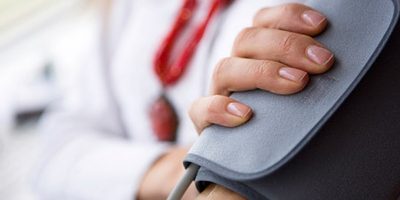
A multi-disciplinary team led by The George Institute’s Professor Alta Schutte has been awarded A$5 million over five years to focus on improving the treatment of hypertension, or high blood pressure, a leading cause of premature death and disability.
Australia’s blood pressure control rates of 32% are very poor by international standards - 68% in Canada for example - with no measurable improvements over the last decade. Of the 1.4 billion dollars spent on treatment annually, much comes from patient out-of-pocket fees, and is often directed to low-value care, such as the fee-for-service model. The latter creates financial drivers to maintain the number of services by one professional and discourages the coordination of care across multiples providers, disciplines and settings, which would achieve better health outcomes.
The problem of poor control persists despite unequivocal evidence that blood pressure lowering medication reduces cardiovascular events. One issue is the hesitancy to prescribe or intensify treatment after high readings and ensuring patients keep taking their medication in the long-term. Another is a lack of focus on patients’ needs and on achieving positive patient outcomes.
The multidisciplinary team has developed and identified a range of high-potential treatment interventions which have not been effectively implemented or scaled in Australia. The funding will allow a primary care virtual hypertension registry to be established that will help researchers evaluate selected interventions against the following criteria - acceptability to providers and patients; cost-effectiveness, and whether they are scalable across the country.
The first trial to be conducted using the registry will focus on the contentious issue of prescription duration which has recently changed from one month to two months in Australia. The trial will focus on even longer prescription durations because they are likely to be much more cost-effective and to improve adherence (thus better at lowering blood pressure) in people with stable hypertension.
Prof Schutte said that this aspect alone has the potential to lead to cost savings of over A$100 million annually.
“The result will be substantially improved health and economic outcomes – since high blood pressure causes 25,000 premature deaths per year and the economic impact of lost productivity is over $90 billion over a working lifetime,” she said.